No cure has yet been found for ALS. However, there are treatments available that can
help control symptoms, prevent unnecessary complications, and make living with the disease easier.
Supportive care is best provided by multidisciplinary teams of health care professionals such as
physicians; pharmacists; physical, occupational, and speech therapists; nutritionists; social workers; respiratory therapists and clinical psychologists;
and home care and hospice nurses. These teams can design an individualized treatment plan and provide special equipment aimed at keeping people
as mobile, comfortable, and independent as possible.
We can classify these treatments into certain sectors:

The U.S. Food and Drug Administration (FDA) has approved the drugs riluzole (Rilutek) and edaravone (Radicava) to treat ALS.
Riluzole is believed to reduce damage to motor neurons by decreasing levels of glutamate, which transports messages between nerve cells and motor neurons.
Clinical trials in people with ALS showed that riluzole prolongs survival by a few months, particularly in the bulbar form of the disease,
but does not reverse the damage already done to motor neurons. Edaravone has been shown to slow the decline in clinical assessment of daily functioning in persons with ALS.
Physicians can also prescribe medications to help manage symptoms of ALS, including muscle cramps, stiffness, excess saliva and phlegm,
and the pseudobulbar affect (involuntary or uncontrollable episodes of crying and/or laughing, or other emotional displays).
Drugs also are available to help individuals with pain, depression, sleep disturbances, and constipation.
Pharmacists can give advice on the proper use of medications and monitor a person’s prescriptions to avoid risks of drug interactions.
Physical therapy and special equipment can enhance an individual’s independence and safety throughout the course of ALS. Gentle, low-impact aerobic exercise such as
walking, swimming, and stationary bicycling can strengthen unaffected muscles, improve cardiovascular health, and help people fight fatigue and depression.
Range of motion and stretching exercises can help prevent painful spasticity and shortening (contracture) of muscles.

Physical therapists can recommend exercises that provide these benefits without overworking muscles.
Occupational therapists can suggest devices such as ramps, braces, walkers, and wheelchairs that help individuals conserve energy and remain mobile.
People with ALS who have difficulty speaking may benefit from working with a speech therapist, who can teach adaptive strategies to speak louder and more clearly.
As ALS progresses, speech therapists can help people maintain the ability to communicate. They can recommend aids such as computer-based speech synthesizers that
use eye-tracking technology and can help people develop ways for responding to yes-or-no questions with their eyes or by other nonverbal means.

Some people with ALS may choose to use voice banking while they are still able to speak as a process of storing their own voice for future use in computer-based speech synthesizers.
These methods and devices help people communicate when they can no longer speak or produce vocal sounds.
Nutritional support is an important part of the care of people with ALS. It has been shown that individuals with ALS will get weaker if they lose weight.
Nutritionists can teach individuals and caregivers how to plan and prepare small meals throughout the day that provide enough calories, fibre, and fluid and
how to avoid foods that are difficult to swallow. People may begin using suction devices to remove excess fluids or saliva and prevent choking.
When individuals can no longer get enough nourishment from eating, doctors may advise inserting a feeding tube into the stomach.
The use of a feeding tube also reduces the risk of choking and pneumonia that can result from inhaling liquids into the lungs.
As the muscles responsible for breathing start to weaken, people may experience shortness of breath during physical activity and difficulty breathing at night or when lying down.
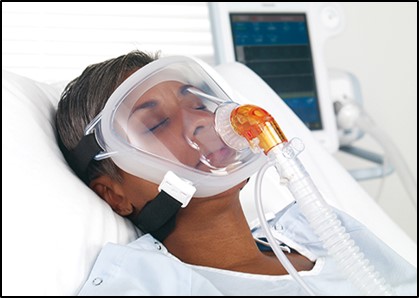
Doctors may test an individual’s breathing to determine when to recommend a treatment called non-invasive ventilation (NIV).
NIV refers to breathing support that is usually delivered through a mask over the nose and/or mouth. Initially, NIV may only be necessary at night.
When muscles are no longer able to maintain normal oxygen and carbon dioxide levels, NIV may be used full-time.
NIV improves the quality of life and prolongs survival for many people with ALS.
Because the muscles that control breathing become weak, individuals with ALS may also have trouble generating a strong cough.
There are several techniques to help people increase forceful coughing, including mechanical cough assist devices and breath stacking.
In breath stacking, a person takes a series of small breaths without exhaling until the lungs are full, briefly holds the breath, and then expels the air with a cough.
As the disease progresses and muscles weaken further, individuals may consider forms of mechanical ventilation (respirators) in which a machine inflates and deflates the lungs.
Doctors may place a breathing tube through the mouth or may surgically create a hole at the front of the neck and insert a tube leading to the windpipe (tracheostomy).
The tube is connected to a respirator.

Individuals with ALS and their families often consider several factors when deciding whether and when to use ventilation support. These devices differ in their effect on a person’s quality of life and in cost. Although ventilation support can ease problems with breathing and prolong survival, it does not affect the progression of ALS. People may choose to be fully informed about these considerations and the long-term effects of life without movement before they make decisions about ventilation support.