The cause of ALS is not known, and scientists do not yet know why ALS strikes some people and not others.
However, evidence from scientific studies suggests that both genetics and environment play a role in the development of ALS.
An important step toward determining ALS risk factors was made in 1993 when scientists supported by
the National Institute of Neurological Disorders and Stroke (NINDS) discovered that mutations in the SOD1 gene were associated with some cases of familial ALS.
Although it is still not clear how mutations in the SOD1 gene lead to motor neuron degeneration, there is increasing evidence that the gene playing a role in.
It is estimated that 5 to 10% of all ALS cases are due to an inherited genetic mutation, often in the superoxide dismutase 1 (SOD1) gene.
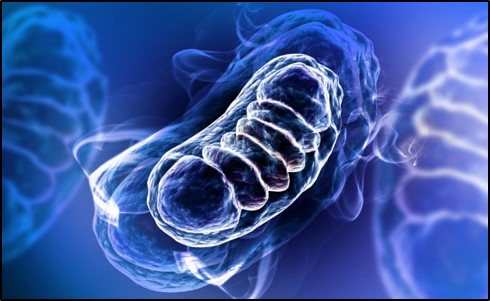
This gene encodes a key protein important for the detoxification of motor neurons. SOD1 is found in the neuron’s mitochondria, small organelles where cellular energy is produced.

“About 90 percent of the energy in the brain is generated by mitochondria,” said the study’s senior author Dr. Zu-Hang Sheng in a news release.
“If the mitochondria aren’t healthy, they produce energy less efficiently; they can also release harmful chemicals called reactive oxygen species that cause cell death.
As a consequence, mitochondrial damage can cause neurodegeneration.”
Since then, more than a dozen additional genetic mutations have been identified, many through NINDS-supported research, and each of these
gene discoveries is providing new insights into possible mechanisms of ALS.
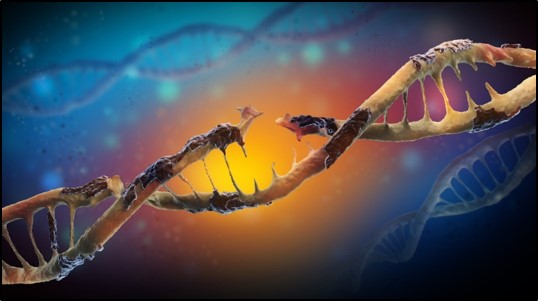
The discovery of certain genetic mutations involved in ALS suggests that changes in the processing of RNA molecules may lead to
ALS-related motor neuron degeneration. RNA molecules are one of the major macromolecules in the cell involved in directing
the synthesis of specific proteins as well as gene regulation and activity.
Other gene mutations indicate defects in the natural process in which malfunctioning proteins are broken down and used to build new ones, known as protein recycling.
Still others point to possible defects in the structure and shape of motor neurons, as well as increased susceptibility to environmental toxins.
Overall, it is becoming increasingly clear that a number of cellular defects can lead to motor neuron degeneration in ALS.
In 2011 another important discovery was made when scientists found that a defect in the C9ORF72 gene is not only present in
a significant subset of individuals with ALS but also in some people with a type of frontotemporal dementia (FTD).
This observation provides evidence for genetic ties between these two neurodegenerative disorders. Most researchers now believe ALS and some forms of FTD are related disorders.
In searching for the cause of ALS, researchers are also studying the impact of environmental factors. Researchers are investigating
a number of possible causes such as exposure to toxic or infectious agents, viruses, physical trauma, diet, and behavioural and occupational factors.
For example, researchers have suggested that exposure to toxins during warfare, or strenuous physical activity,
are possible reasons for why some veterans and athletes may be at increased risk of developing ALS.
Although there has been no consistent association between any environmental factor and the risk of developing ALS, future research may show that some factors are involved in the development or progression of the disease.